- Homepage
- Research
- Research groups & Laboratories
- Infection immunology
Research Projects
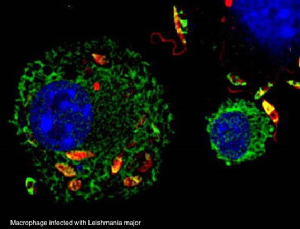
Our lab focuses on studying skin immune responses against infections. We mainly utilize the model of cutaneous leishmaniasis, initiated by parasitic infections with Leishmania major. Current projects concentrate on studying the Dendritic cell (DC) subtypes involved in defense mechanisms, the interaction of DC with T cells (antigens recognized, T cell subsets involved), and the role of additional myeloid cells for immune regulation (mast cells, monocytes/macrophages). The involvement of innate lymphoid cells (ILC) in protection against leishmaniasis as well as inflammasome-dependent cell death in skin defense are equally addressed in our investigations.
Using so-called 'humanized mouse models', translation of basic research findings into the clinical setting is central. Deciphering the details of immunity against the parasite will aid not only basic research in skin immunity against various pathogens and in chronic inflammatory processes but will also promote the development of a vaccine against this important human pathogen.
Understanding the immunological control of inflammatory skin diseases in humans, triggered among other reasons by pathologically activated T cell response in humans, concerns us further in diverse projects addressing e.g. atopic dermatitis, psoriasis vulgaris, graft-versus-host reaction and hidradenitis suppurativa ultimatively leading to further testings in clinical studies.
Ngouateu Tateng A, Ngouateu OB, Khan Payne V, Maurer M, von Stebut E, Krüger A, Dondji B. Ecological site distribution of sand fly species of Mokolo, an endemic focus of cutaneous leishmaniasis in northern Cameroon. Acta Trop. 2023 Mar;239:106809.
Demircik F, Kostka SL, Tenzer S, Waisman A, von Stebut E. Cross reactive, natural IgG recognizing L. major promote parasite internalization by dendritic cells and promote protective immunity. J Mol Med (Berl). 2022 Mar;100(3):461.
Yogev N, Bedke T, Kobayashi Y, Brockmann L, Lukas D, Regen T, Croxford AL, Nikolav A, Hövelmeyer N, von Stebut E, Prinz M, Ubeda C, Maloy KJ, Gagliani N, Flavell RA, Waisman A, Huber S. CD4+ T-cell-derived IL-10 promotes CNS inflammation in mice by sustaining effector T cell survival. Cell Rep. 2022 Mar 29;38(13):110565. doi: 10.1016/j.celrep.2022.110565.
Lopez Kostka S, Kautz-Neu K, Yogev N, Lukas D, Holzmann B, Waisman A, Clausen BE, von Stebut E. Exclusive Expression of MyD88 on Dendritic Cells Is Lopez Kostka Sufficient to Induce Protection against Experimental Leishmaniasis. J Invest Dermatol. 2021 Sep 24:S0022-202X(21)02216-8.
https://doi.org/10.1016/j.jid.2021.07.184
de Freitas E Silva R, von Stebut E. Unraveling the Role of Immune Checkpoints in Leishmaniasis. Front Immunol. 2021 Mar 11;12:620144.
https://www.frontiersin.org/articles/10.3389/fimmu.2021.620144/full
Lukas D, Dietze-Schwonberg K, Kautz-Neu K, Lorenz B, Yogev N, Clausen BE, von Stebut E. Induction of Regulatory T Cells in Leishmania major‒Infected BALB/c Mice Does Not Require Langerin+ Dendritic Cells. J Invest Dermatol. 2021 Apr;141(4):936-938.
von Stebut E, Boehncke WH, Ghoreschi K, Gori T, Kaya Z, Thaci D, Schäffler A. IL-17A in Psoriasis and Beyond: Cardiovascular and Metabolic Implications. Front Immunol. 2020 Jan 15;10:3096.
https://www.frontiersin.org/articles/10.3389/fimmu.2019.03096/full
von Stebut E, Reich K, Thaçi D, Koenig W, Pinter A, Körber A, Rassaf T, Waisman A, Mani V, Yates D, Frueh J, Sieder C, Melzer N, Mehta NN, Gori T. Impact of Secukinumab on Endothelial Dysfunction and Other Cardiovascular Disease Parameters in Psoriasis Patients over 52 Weeks. J Invest Dermatol. 2019 May;139(5):1054-1062.
https://reader.elsevier.com/reader/sd/pii/S0022202X1832904X?token=609120879236CBBC972D833C0D69E52F7938C387966A2EBF4CE509DF820B1E90C8C434B4026FBA07522252FE10576E3A&originRegion=eu-west-1&originCreation=20211028104103
Bohn T, Rapp S, Luther N, Klein M, Bruehl TJ, Kojima N, Aranda Lopez P, Hahlbrock J, Muth S, Endo S, Pektor S, Brand A, Renner K, Popp V, Gerlach K, Vogel D, Lueckel C, Arnold-Schild D, Pouyssegur J, Kreutz M, Huber M, Koenig J, Weigmann B, Probst HC, von Stebut E, Becker C, Schild H, Schmitt E, Bopp T. Tumor immunoevasion via acidosis-dependent induction of regulatory tumor-associated macrophages. Nat Immunol. 2018 Dec;19(12):1319-1329.
https://doi.org/10.1038/s41590-018-0226-8
Kautz-Neu K, Noordegraaf M, Dinges S, Bennett CL, John D, Clausen BE, von Stebut E. Langerhans cells are negative regulators of the anti-Leishmania response. J Exp Med. 2011 May 9;208(5):885-91.
https://rupress.org/jem/article-pdf/208/5/885/1131952/jem_20102318.pdf